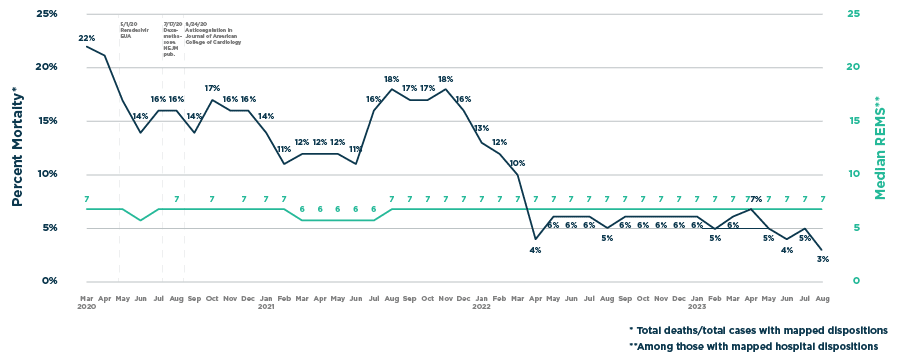
Mortality Rate and Acuity of Hospitalized COVID-19 EMS Patients
EMS COVID-19 and Influenza-like Illness Surveillance
911 Records with COVID-19 EMS Provider Impressions
911 Records with COVID-19 ED or Hospital Diagnoses
COVID-19 Deaths: EMS 911 Transports
911 Records with Influenza-like Illness (ILI) EMS Provider Impressions
Flu and RSV Infection Rate
Flu Diagnoses
RSV Diagnoses
Limitations
*This page will be updated daily Monday through Friday. Data are published with a 48-hour delay to allow adequate time for providers to complete and lock records.
The following reports include records with an EMS provider primary or secondary impression of:
COVID-19 – Confirmed by testing
COVID-19 – Exposure to confirmed patient
COVID-19 – Suspected – no known exposure
Because these reports are based on EMS provider impression and information available in the out-of-hospital setting, these records may or may not represent confirmed COVID-19 cases.